Anal Fistula: Symptoms, Causes, Treatment, Surgery and Recovery
Posted in :
Dealing with pain, swelling, or discharge near the anus can feel uncomfortable to talk about, but these symptoms are more common than many people realize. If you are worried about an anal fistula, understanding what it is and how it is treated can help you take the next step with more confidence.
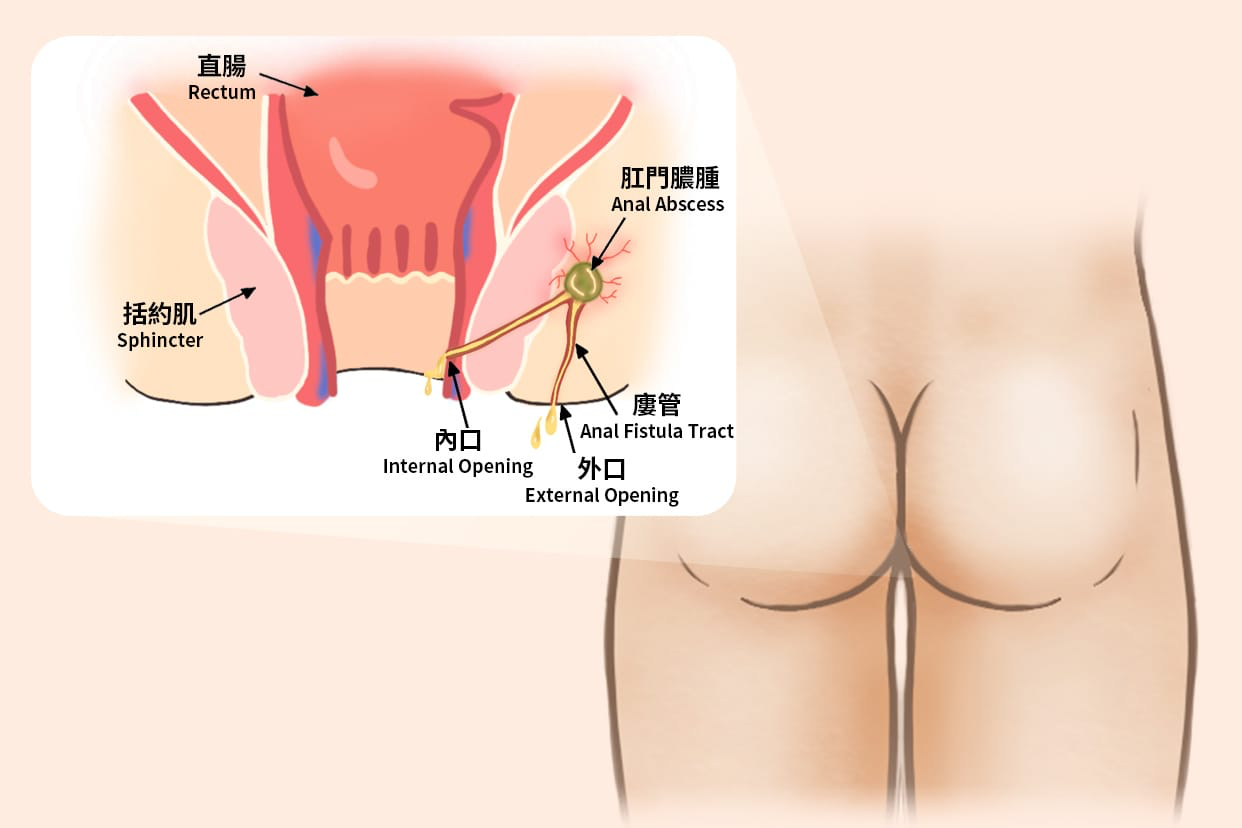
An anal fistula is a small tunnel that forms between the inside of the anal canal and the skin near the anus. It often develops after an infection in an anal gland causes an abscess, and after the abscess drains, a passage may remain under the skin.
What is an anal fistula?
An anal fistula, also called fistula-in-ano, is an abnormal connection between the inside of the anus and the outer skin. Most anal fistulas are related to a previous anal abscess, and they are usually considered a chronic problem unless treated properly.
This condition is different from hemorrhoids or anal fissures. Hemorrhoids are swollen veins, and fissures are small tears in the lining of the anus, while an anal fistula is usually linked to infection and a tract beneath the skin.
Anal fistula symptoms
Anal fistula symptoms can be mild at first, but they often become more noticeable over time. Common symptoms include:
- Pain around the anus, especially when sitting, walking, or passing stool.
- Swelling, redness, or tenderness near the anus.
- Pus or foul-smelling discharge from an opening near the anus.
- Skin irritation around the anal area.
- Bleeding in some cases.
- Fever or general illness if infection is still active.
Many people notice a repeating pattern where the area swells, drains, feels better for a while, and then flares up again. That cycle can be a sign that an abscess has turned into a fistula.
What causes an anal fistula?
The most common cause of an anal fistula is an infection in one of the small glands inside the anus. When the gland becomes blocked, it can lead to an abscess, and once that abscess drains, a tunnel may remain.
Other related causes or risk factors can include Crohn’s disease, diverticulitis, hidradenitis suppurativa, tuberculosis, HIV, previous surgery, or trauma in the area. In rare cases, anal fistulas may also be linked to cancer or radiation damage.
Does an anal fistula heal on its own?
In most cases, no. Anal fistulas generally do not heal by themselves, and surgery is often needed to remove the tract, control infection, and reduce the risk of the problem returning.
This is why home remedies alone are usually not enough. Warm baths may ease discomfort, but they do not close the fistula tunnel.
How is anal fistula diagnosed?
Doctors usually begin with a review of symptoms and an examination of the area. In some cases, they may recommend additional testing to understand the exact path of the fistula and to choose the safest treatment.
A proper diagnosis matters because an anal fistula can sometimes be mistaken for hemorrhoids, fissures, or a recurring abscess. The right diagnosis helps avoid delayed treatment and repeated infections.
Anal fistula treatment options
•Fistulotomy, where the tract is opened so it can heal flat, often used for simpler fistulas.
•Seton placement, where a surgical thread is placed through the fistula to allow drainage and protect the sphincter muscle.
•Advancement flap, where tissue is used to cover the internal opening after repair.
•Other procedures, such as the LIFT technique, plugs, glue, or newer specialist approaches in selected cases.
The best procedure depends on your specific fistula. A colorectal surgeon usually decides this based on complexity and the risk to continence.
Anal fistula surgery recovery
Recovery after anal fistula surgery varies depending on the type of procedure and the size of the wound. Some people return to normal activity within a few days, while full healing may take several weeks.
Final thoughts
Anal fistula can be painful and frustrating, but it is treatable. If your symptoms keep coming back or you notice drainage, swelling, or pain near the anus, it is important to get checked by a qualified healthcare professional.
Medical disclaimer:
This article is for informational purposes only and is not a substitute for professional medical advice, diagnosis, or treatment. Always speak with a qualified healthcare provider about your symptoms